'Missing episodes' add to elective surgery backlog
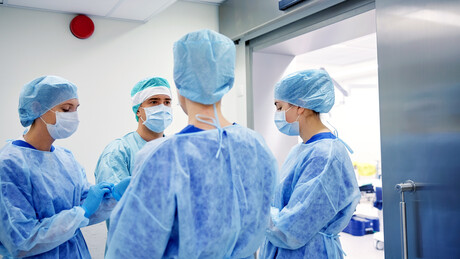
A sharp increase in ‘missing episodes’ of care in Australia’s private hospitals in the first quarter of 2022 spells longer waits for essential elective surgery.
The latest data from the Australian Prudential Regulation Authority (APRA) suggests that since the start of the pandemic more than 390,000 anticipated admissions to private hospitals did not occur. Over 100,000 of these ‘missing episodes’ were added in the first three months of 2022 alone, further increasing elective surgery wait times. This means all the gains made in 2021 in terms of elective surgery catch-up have been wiped out and surgical waiting lists are longer than they have ever been, according to APHA.
APHA CEO Michael Roff said every state had elective surgery restrictions in place over this quarter, contributing further to already extensive backlogs.
“The Omicron wave resulted in surgery restrictions being imposed right around the country in the first quarter of 2022 and these figures show the devastating impact of that action,” he said.
In addition, although the number of private patients treated in public hospitals has fallen, the proportion remains the same, with public hospitals undertaking 15% of privately insured episodes.
“This means public hospitals have not prioritised clearing the backlog of public patients on ever-growing waiting lists who need their care most, but are continuing to chase private health insurance revenue at the expense of public patients.
“This will weigh heavily on patients who are left waiting for non-urgent, but necessary surgery.”
The number of Australians taking up hospital cover continues to increase, with an additional 225,858 joining in the last 12 months.
“While it is encouraging to see Australians recognising the value of private hospitals in providing them high-quality care when they need it, the health workforce crisis will make it challenging to deliver all the elective surgery needed in the coming year,” Roff said.
“In addition to increased staff absenteeism due to COVID, private hospitals have told us they currently have a shortfall of 5500 nurses and they urgently need at least 1000 skilled migrant nurses. The incoming federal government’s first task should be addressing the health workforce crisis in Australia by making this country an attractive option to skilled migrants.”
He said Australia was up against fierce international competition when it comes to recruiting health professionals — particularly nurses — and a business-as-usual approach will not be enough to bring them here.
“The difficulty we have recruiting is not just about money, people want to immigrate to a place where they will be welcomed and there is an opportunity to settle with their family. The UK, Canada and France are all offering enhanced residency pathways for healthcare workers who choose to move there, and Australia needs to follow suit.
“In addition, removing bureaucratic red tape imposing unnecessary restrictions on employers and visa holders needs to be addressed to allow for a more flexible health workforce.
“Addressing health workforce shortages will be the first and most important issue we raise when we meet with the new health minister,” Roff said.
Australia invests further $14.6 million in national allergy research
Further funding until June 2028 for the National Allergy Centre of Excellence (NACE) and the...
Balcony and nearby construction activities linked to RPA deaths
The investigation report into the Royal Prince Alfred Hospital fungal outbreak that occurred in...
$1bn vaccine and antivenom manufacturing facility opens
A $1 billion cell-based influenza vaccine and antivenom manufacturing facility has opened in...




![[New Zealand] Transform from Security Awareness to a Security Culture: A Vital Shift for SMB Healthcare — Webinar](https://d1v1e13ebw3o15.cloudfront.net/data/89856/wfmedia_thumb/..jpg)
![[Australia] Transform from Security Awareness to a Security Culture: A Vital Shift for SMB Healthcare — Webinar](https://d1v1e13ebw3o15.cloudfront.net/data/89855/wfmedia_thumb/..jpg)



