A crystal clear answer for pressure injury prevention and management
Thursday, 20 March, 2014
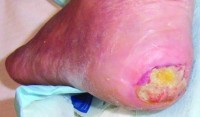
The Pressure Injury Prevention Program in the Hunter New England Health Local Health District is a model highly recognised within the healthcare profession since its inception in 2008. The program’s clinical lead Margo Asimus, nurse manager Felicity Williams and project officer Pui Ling (Iris) Li explain the program’s aims and outcomes.
It is 2014 and pressure injuries continue to remain a major problem for patients, families, health care professionals and organisations 1. This adverse event contributes to harm of patients which affects long term wellbeing, while increasing length of stays2 and placing additional demands on the health care budget. An organisation that is willing to address this predominately avoidable injury must firstly be prepared to measure the real extent of the problem. It is then that the necessary strategies and changes can be implemented.
Pressure injury point prevalence studies have been performed in five states across Australia; Victoria, Queensland, Tasmania, Western Australia and ACT. In 2003, 2004 and 2006 the Victorian Quality Council (VQC) supported point prevalence studies which resulted in significant improvement in prevalence rates from 26 per cent in 20033 to 17.6 per cent by 20064 . The state of Western Australia commenced state wide auditing in 2007 which has continued through the WoundsWest program (WoundsWest)5. WA identified improvement strategies which also resulted in the reduction in the hospital acquired prevalence rates.
In an effort to gain continual improvement in reducing hospital acquired pressure injury prevalence rates, Queensland has imposed financial penalties for both stage 3 ($30,000) and 4 pressure injuries ($50,000) which had been classified as an adverse event.

Jackson et al (2011)6 reviewed the ICD10 coder data for hospital acquired conditions from 2006 to 2007 in public hospitals in the states of Victoria and Queensland. Over 144 categories were determined with pressure injuries being in the top 10 of all adverse events, (5th place) with over 2,873 cases identified in the 12 month period. The cost of a hospital acquired pressure injury was calculated at on average $8,435 for each case. It also reported an estimated expenditure of $24,234,740 would be required in the health care budget to treat the complications of a pressure injury.
The increasing pressure injury prevalence, patient harm and escalating health care costs prompted an urgent organisational change to improve the quality and safety of care within a large health service in NSW1. A systematic approach to pressure injury prevention and management was implemented with outstanding achievements in several key areas.
Crystal Model: A Crystal Clear Solution for Pressure Injuries
The Crystal Model was developed by Hunter New England Local Health District (HNELHD) in NSW and has been implemented by the Pressure Injury Prevention Program (PIPP) at an executive level in HNELHD7. It has focused on the prevention and management of pressure injuries since 2008; the prevalence rate of hospital-acquired pressure injuries decreased by13.5 per cent over the six years. This Model has been recognised as best practice by winning the Clinical Excellence Commission Award in the 2009 at the NSW Health Baxter Awards.

There are nine components in the Crystal Model, which are interconnected in prevention and management of pressure injuries– policy, surveillance, equipment, communication, documentation, wound management, education, paediatrics and community care. Each component has a leader, a clinician or manager who has substantive roles in the PIPP and promotes the development of resources and strategies.
Figure 1: Crystal Model Diagram
HNELHD Pressure Injury Prevention Program Crystal Model: A range of key aspects working together to stop pressure injuries
Crystal Model Components
Policy
The Pressure Injury Prevention and Management Policy include an equipment algorithm and have been developed with the reference to the best practice guideline. The policy interconnects key focus areas, strategies and evidence. The policy is reviewed regularly following recommendations from recent pressure injury prevalence studies.
 Surveillance
Surveillance
Annual point prevalence surveys should be conducted to identify pressure injury prevalence, the sources and severity of the pressure injuries, patients’ risk profile of pressure injury and current prevention and management strategies. Our project has demonstrated that annual surveillance provides evidence of the effectiveness of strategies implemented, informs the development of future strategies, and enables future benchmarking.
Equipment
Appropriate choice of pressure redistributing equipment is one of the important components in pressure injury prevention. In HNELHD, an equipment algorithm has been developed and implemented alongside an agreed and validated risk assessment tool8.The algorithm guides clinicians to identify through risk assessment the most appropriate pressure redistributing device.
Communication
The pressure injury prevention program logo was established as a marketing strategy. The communication strategies include fact sheets, meetings, and a dedicated PIPP website to ensure that all information and resources about the Pressure Injury Prevalence Study were supplied promptly to managers, staff and patients. In addition, all study results together with recommendations are accessible on the PIPP website.
Documentation
Introduction and implementation of a validated pressure injury risk assessment tool, Waterlow Risk Assessment8 and Pressure Injury Notification Sticker enables Incident Information Management System (IIMS) and coder data to be compared. This information provides clinical units with direction to improve clinical care and documentation. Incidents of pressure injuries are expected to be reported to the IIMs of the health organisation for analysis of the root cause of the adverse event which then informs improvement strategies.
Education
An interactive online program has been developed, which is available to all clinicians and students across HNELHD. The purpose of the program is to provide accessible, consistent training, develop knowledge and critical thinking about pressure injury prevention, assessment and management. Completion requires successfully undertaking of an on-line assessment that is automatically recorded on the staff member’s learning record. Evaluation of the validity of the knowledge acquisition and competence was undertaken during the initial pilot of the on-line education evaluated.
Wound management
Evidence-based management of pressure injuries using wound management principles has been implemented and this information is provided within an e-learning program.
Paediatrics and Community
PIPP community study has identified gaps in pressure injury prevention in clients living in the community9. Strategies have been introduced to prevent pressure injuries following patients’ discharge into the community settings. The paediatric population has specific care needs that now form part of specific care delivery to avoid pressure damage from device related pressure.
Measuring the extent of the pressure injuries Prevalence studies and clinic audits should be conducted to measure the extent of the organisations pressure injury problem and the effectiveness of the PIPP implemented. Also, to demonstrate excellence in accreditation, the systems such as prevalence study, clinical coder audit and IIMS data management that can capture, analyse and report data outcomes should be demonstrated.
“There are nine components in the Crystal Model, which are interconnected in prevention and management of pressure injuries – policy, surveillance, equipment, communication, documentation, wound management, education, paediatrics and community care.”
 Prevalence vs Incidence
Prevalence vs Incidence
The proportion of patients with a pressure injury(s) within a particular population at a given time is known as pressure injury prevalence; and the number of patient with a new pressure injury (s) in a specified population during a period of time is known as incidence. The prevalence study reflects the magnitude of the problem, while the incidence study reveals the quality of care provided. 10
Data content
Apart from patients’ demographics, the sources: hospital acquired or pre-existing, severity and anatomical locations of the pressure injuries, the following data can also be collected to assess the awareness of pressure injury prevention:
- Compliances in risk and skin assessment and reassessment
- Preventative action taken
- Appropriateness of the supporting surface and the length of time to access pressure redistributing equipment, especially for community clients
- Compliances in IIMs reporting
The extent of data this collected will also depend on the purpose of the study and resources available, such as the number of surveyors, number of eligible patients to be surveyed, settings ( inpatient or community), and who will manage the data. The quality of analysis can also be affected by available resources.
Planning and study methodology
At HNELHD it has been necessary to obtain ethics approval before conducting the district wide annual study. The methodology of the study has been determined to collect accurate, valid and consistent data collection to enable trending, benchmarking and comparison with other studies
The point prevalence study can be conducted, for example, by physical examination and medical record audit and extracting data from clinical record coding or IIMs. It also sets out explicitly the inclusion and exclusion criteria, such as age, ward, and medical specialty. The methodology of the study in acute settings varies from primary care settings.
Validity of the study
To ensure the quality of data collected, standardised education and training and inter-rater testing are required for surveyors prior to the prevalence study11. An external assessor or independent surveyor is allocated to each survey team to mitigate bias.
HNELHD first point prevalence surveillance conducted in 2008 survey was facilitated by the district project team members leading surveillance teams. Local ownership of annual surveillance has transitioned as surveyors were trained and assessed. PIPP district team members were able to support surveillance teams by providing education and validation regarding the methodology and process to facilitate that the survey is consistent and of appropriate.
As the study with higher consent rate is more likely to reflect the true prevalence rate of pressure injuries, all facilities in HNELHD are required to achieve a minimum of 75% consent rate for eligible patients in prevalence studies.
Leadership has been a crucial component of the program’s success12. Executive sponsorship by the District Director of Nursing and Midwifery was vital in recognising the role of nurses in identifying risk, preventing and managing pressure injuries. Executive sponsorship has engaged strategic and clinical leaders responsible for implementation of standardised prevention and management. The clinical governance unit are engaged and involved to enable pressure injury prevention to interface with other district wide programs. A range of forums have been used to convey a consistent message to staff at all levels of the organisation these focus on clinical quality and patient care and include Senior Nurse Management, executive leadership and Nurse Educators/Nurse Practitioner/Clinical Nurse Consultant forums. They provide opportunity for the Pressure Injury project team to report on key results and trends emerging from prevalence studies and engage with staff on strategies for improvement.
The interdisciplinary district project team consists of members from clinical nursing, allied health and management with medical staff contributing to sub-committee activities as key stakeholders. Membership is based on geographical location, clinical expertise and ability to influence and lead1. The team is responsible for the development of processes, policies, procedures and engaging content matter experts around current evidence based practice to prevent and manage pressure injuries.
To cascade a consistent message to 41 inpatient facilities and 44 community health centres, Pressure Injuries has been included as a KPI for clinical managers. This factor facilitates engagement and clarifies accountability for clinicians at all levels of the organisation in preventing adverse events. The Pressure Injury prevention and management e-Learning program interfaces with the district learning management system (LMS). All clinicians who prescribe pressure relieving/ redistributing equipment are required to undertake the learning program and managers have access to their staff completion details. The online PI learning course is required by all people who participate as a surveyor.
Following the first district wide point prevalence study a mattress replacement scheme and equipment algorithm were rolled out. Hiring of powered mattress systems was reduced and this saved $500,000 in the first year. The reduction in preventable pressure injury prevalence and severity has also reduced the cost of services by contributing to reducing use of consumables and reducing length of stay
The annual point prevalence surveillance is the key evaluation process for implementation of pressure injury prevention and management strategies. Analysis of trends informs the priorities and direction that future strategies should take. To undertake the survey in all 44 inpatient facilities, the commitment of approximately 200 staff members is required.
Survey teams of three people consist of all levels of nursing, from undergraduate students, local university academic staff to senior nursing leaders. Inter-disciplinary engagement has occurred with increasing numbers of allied health participating in these teams.
The Pressure Injury project team analyses the data and prepares reports for the district, clusters, facilities and wards. Accompanying these are survey recommendations which are individualised according to the results. The reports are pivotal to the communication process and are published on the intranet site so all managers can compare results with other services.
In recent years alignment with the clinical governance unit has been strengthened by the inclusion of Pressure Injuries in the National Safety and Quality Health Service (NSQHS) Standards as Standard 813. The district uses a range of change management strategies to cascade strategies, articulate accountabilities and imbed expected behaviours.
The Crystal model developed in HNELHD is an example of a systematic approach which engages both executive leadership and clinicians in the prevention and management of pressure injuries. Implementing the best practice strategies has created a difference in the quality and safety for those patients in our care.
Additional resources are now available to support organisations in developing programs to minimise the prevalence of pressure injuries. In 2012 the Pan Pacific Clinical Practice Guideline for the Prevention and Management of Pressure Injury8 were released and can be freely accessed on the Australian Wound Management Association website (http://www.awma.com.au/publications/publications.php#pipm ). These guidelines have been acknowledged across Australia as a best practice resource for organisations to refer to in preparation to meet National standards, improve outcomes and reduce the incidence of this avoidable wound.
“Prevalence studies and clinic audits should be conducted to measure the extent of the organisations pressure injury problem and the effectiveness of the PIPP implemented.”
Margo Asimus is a Nurse Practitioner - Wound Management and Clinical Lead (2008-2013) for the Pressure Injury Prevention Program in the Hunter New England Health Local Health District. She participated in the guideline development group for the Pan Pacific Clinical Practice Guideline for the Prevention and Management of Pressure Injury. Margo is Vice President of the Australian Wound Management Association (AWMA) and President of AWMA-NSW.
Felicty Williams is the Nurse Manager Professional Development for HNELHD. She has additional Midwifery and Management qualification and broad experience across Metropolitan, Rural and Remote Nursing. She has management responsibilities for the Pressure Injury Prevention Program at HNHELHD since 2008 and education component at a local and state level.
Pui Ling (Iris) Li currently works as a Project Officer. She has been involved in the Pressure Injury Prevention Program since 2009. Iris completed her nursing Gerontic Master degree in 2005.
REFERENCES
1. Asimus M, Maclellan L, Li P. Pressure ulcer prevention in Australia: the role of the nurse practitioner in changing practice and saving lives. Int Wound J. 2011;8(5):508–13.
2. Graves N, Birrell F, Whitby M. Effect of pressure ulcer on length of hospital stay. Infect Control Hosp Epidemiol. 2005;26(3):293–7.
3. Victoria Quality Council VQC State-wide PUPPS Report-2003 [Internet]. Victoria; Department of Human Services; 2004 [cited 21/1/2014] Available from: http://www.health.vic.gov.au/qualitycouncil/downloads/pupps2/statepupps_ report.pdf
4. Victorian Quality Council VQC State-wide PUPPS Report 2006. [Internet]. Victoria; Department of Human Services; 2007 [cited 21/1/2014] Available from: http://www.health.vic.gov.au/pressureulcers/downloads/pupps3.pdf
5. Strachan V., Prentice J., Newall N., Elmes R., Carville K., Santamaria N. & Della P. WoundsWest Wound Prevalence Survey 2007 State-wide Report. Ambulatory Care Services, Department of Health 2007: Perth, Western Australia.
6. Jackson, T., Nghiem, H.S., Rowell, D., Jorm, C. & J. Wakefield ‘Marginal costs of hospital acquired diagnoses: Information for priority setting for patient safety programs and research,’ Journal of Health Services Research &Policy, 2011. 16(3): 141-146.
7. Rayner R, Asimus M, Li PL. Pressure Injury. In: Swanson T, Asimus M, McGuiness B editors. Wound Management for the Advanced Practitioner. 1st ed. London: Academic Press; In Press May 2014.
8. Australian Wound Management Association. Pan Pacific Clinical Practice Guideline for the Prevention and Management of Pressure Injury. Cambridge Media Osborne Park, WA: 2012
9. Asimus M, Li P. Pressure ulcers in home care settings: is it overlooked? Wound Practice and Research. 2011: 19(2): 88-97.
10. International guidelines. Pressure ulcer prevention: prevalence and incidence in context. A consensus document. Australia: IP Communications, 2014.
11. Prentice JL, Stacey MC, Lewin G. An Australian model for conducting pressure ulcer prevalence surveys. Primary Intention. 2003;11(2):87–109.
12. Studer Group. The Nurse Leader Handbook, Florida: First Starter Publishing; 2010.
13. Australian Commission on Safety and Quality in Health Care. Safety and Quality Improvement Guide Standard 8: Preventing and Managing Pressure Injuries (October 2012). Sydney. ACSQHC, 2012.
Australia invests further $14.6 million in national allergy research
Further funding until June 2028 for the National Allergy Centre of Excellence (NACE) and the...
Balcony and nearby construction activities linked to RPA deaths
The investigation report into the Royal Prince Alfred Hospital fungal outbreak that occurred in...
$1bn vaccine and antivenom manufacturing facility opens
A $1 billion cell-based influenza vaccine and antivenom manufacturing facility has opened in...




![[New Zealand] Transform from Security Awareness to a Security Culture: A Vital Shift for SMB Healthcare — Webinar](https://d1v1e13ebw3o15.cloudfront.net/data/89856/wfmedia_thumb/..jpg)
![[Australia] Transform from Security Awareness to a Security Culture: A Vital Shift for SMB Healthcare — Webinar](https://d1v1e13ebw3o15.cloudfront.net/data/89855/wfmedia_thumb/..jpg)



