1 in 4 joint replacement surgeries unnecessary
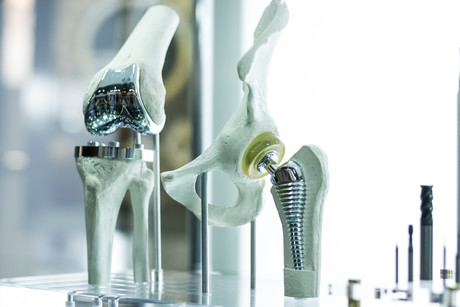
An estimated one in four joint replacement surgeries for people with osteoarthritis (OA) are unnecessary, according to a new report.
In 2016, nearly 100,000 Australians received joint replacements to treat OA of the hip or knee — at an estimated cost of over $2 billion. Between 1994–2014, the state of Victoria had a 175% increase in hip replacements and 285% increase in knee replacements, with no sign of demand slowing.
A major new report into OA in Victoria has suggested a new ‘Model of Care for Osteoarthritis of the Hip and Knee’, which would save money and improve outcomes for many patients. The report, published by MOVE, the national consumer-based organisation for muscle, bone and joint health, carries a series of recommendations for diagnoses, management and treatment of hip and knee OA in Victoria, which challenge many of the existing practices:
- OA can be diagnosed without X-rays.
- OA can be successfully treated in a majority of cases without surgery.
- Joint replacement surgery should only be a treatment of last resort.
- Pain management can be improved.
Non-surgical management strategies, especially for knee OA, have been identified as a key cost-saving measure that would:
- reduce the demand for knee replacements with savings predicted at $233 million by 2030 for the health system;
- improve workforce participation with an estimated yearly reduction of $9.9 million in welfare payments and increased income tax revenue of $8.4 million per year by 2030.
OA is not just a disease of old age. The majority of people with the condition remain in their prime income-earning years (25–64 years). Current projections suggest that the prevalence of OA in Australia will soar by 41% in coming decades. Unless the healthcare system for people with OA of the hip and knee in Victoria is improved, the current sub-optimal care will continue at significant economic, social and personal cost.
“The evidence clearly tells us we can get better outcomes, more cost effectively, for people suffering from OA,” said Report co-authors Prof Andrew Briggs, from the Victorian Musculoskeletal Clinical Leadership Group, and Carolyn Page, from St Vincent’s Hospital. “OA is not an inevitable part of ageing and there are simple and effective management and prevention strategies that could be deployed at scale across Victoria to reduce the burden of disease and contain the growing pressure on Victoria’s health service.”
Director of Orthopaedic Surgery at St Vincent’s Hospital Prof Peter Choong said some arthritis patients think they need a joint replacement when it’s not required; an education campaign is what’s needed. “Joint replacement surgery provides relief for people with advanced joint disease. For those who don’t need it, surgery can cause more problems than it solves. People need to understand there can be much better ways to treat OA, and surgery should be a last resort,” he said.
Australia invests further $14.6 million in national allergy research
Further funding until June 2028 for the National Allergy Centre of Excellence (NACE) and the...
Balcony and nearby construction activities linked to RPA deaths
The investigation report into the Royal Prince Alfred Hospital fungal outbreak that occurred in...
$1bn vaccine and antivenom manufacturing facility opens
A $1 billion cell-based influenza vaccine and antivenom manufacturing facility has opened in...




![[New Zealand] Transform from Security Awareness to a Security Culture: A Vital Shift for SMB Healthcare — Webinar](https://d1v1e13ebw3o15.cloudfront.net/data/89856/wfmedia_thumb/..jpg)
![[Australia] Transform from Security Awareness to a Security Culture: A Vital Shift for SMB Healthcare — Webinar](https://d1v1e13ebw3o15.cloudfront.net/data/89855/wfmedia_thumb/..jpg)



