Improving care for some of the sickest patients in the hospital: new national standard for emergency laparotomy
By Conjoint Professor Carolyn Hullick FACEM*
Friday, 01 May, 2026

Australia’s first Emergency Laparotomy Clinical Care Standard will help health services develop timely, appropriate and standardised approaches to care that will save lives, Chief Medical Officer at the Australian Commission on Safety and Quality in Health Care writes.
When a patient presents to my emergency department with a stroke in the middle of the night, the care pathways and protocols are clear — and these processes are similar across Australia.
But when a patient’s condition means they may need an emergency laparotomy — one of the most time-critical and high-risk surgeries we see outside of major trauma — there is no such standardised national approach.
Patients with urgent abdominal conditions such as a bowel obstruction, bowel perforation or serious internal bleeding can be among the sickest in the hospital. Many of these patients either have sepsis on presentation or are at high risk of developing it. Delaying surgery, when needed, is highly likely to worsen outcomes and can be catastrophic.
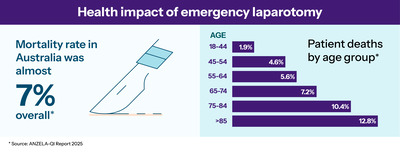
But emergency laparotomy is a complex and high-risk procedure. Though one of the most common emergency surgeries in Australia with more than 15,000 performed each year, it is associated with a mortality rate of around 7%, with estimates as high as 20% in some populations. Older adults, people with frailty or significant comorbidities, and people presenting with sepsis are at particularly high risk.
Recovery from an emergency laparotomy may involve days to weeks in hospital, post-operative complications such as infection and pneumonia, the need for further high-risk interventions, and potential loss of independence for older patients.
Patients who may need an emergency laparotomy, and their families, are confronted with an unexpected and potentially devastating diagnosis for which a positive outcome may not be guaranteed. This means difficult decisions must be made under extreme time pressure, with clinicians they don’t know.
In some cases, surgery may not significantly prolong or improve life, so clinicians must have honest conversations with patients and loved ones about the benefits and risks of surgery and what matters most to the patient.
Despite these complexities, standardised, evidence-based clinical pathways for emergency laparotomy are not embedded in practice in Australia as they are for other time-critical conditions such as stroke or cardiac events, and other surgical emergencies such as hip fracture.
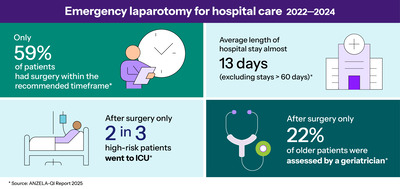
This has led to significant variation in care, for example in timely access to surgery. In cases where a surgeon had recommended surgery within two hours, only 20% reached the theatre in time, according to the latest Australian and New Zealand Emergency Laparotomy Audit – Quality Improvement (ANZELA-QI) report.
The report also showed that access to a consultant surgeon and consultant anaesthetist for operations after hours is inconsistent. Rates of frailty assessment also remain low, and less than a quarter of older emergency laparotomy patients are assessed postoperatively by a geriatrician.
A new national standard of care
Mounting international and Australian evidence shows a structured approach to the care of patients undergoing emergency laparotomy can substantially improve outcomes.
This is why the Australian Commission on Safety and Quality in Health Care (the Commission) has released Australia’s first national Emergency Laparotomy Clinical Care Standard to improve care for patients aged 18 and over undergoing emergency surgery for urgent, high-risk, intra‑abdominal conditions, performed via open or laparoscopic approaches.1
Developed by the Commission with guidance from an expert topic working group, the new Clinical Care Standard describes the care patients should be offered by clinicians and healthcare services throughout Australia.
The Standard provides health professionals with clear guidance on timely recognition and escalation, risk stratification, shared decision-making and the importance of multidisciplinary perioperative care.
It includes quality statements that describe the expected standard for key components of patient care, with explanations of what these mean for patients, clinicians and healthcare services.
Along with the quality statements, the Standard contains a set of clinical indicators that allow health services to monitor care delivery and support implementation of local quality improvement initiatives.
The Standard also addresses specific considerations for patients who may need to be transferred to access investigations or suitable treatment. In regional, rural and remote locations it is essential that systems and networks support timely patient-centred decision-making about transfer, coordination between services and appropriate interventions before transfer.
The best-practice guidance described in the Standard can be distilled into four key elements that make a vital difference to the care received by emergency laparotomy patients. (See Figure 1).
**************************************************
Key takeaways for health services
Evidence shows a systematic approach to emergency laparotomy care — before, during and after surgery — reduces mortality and improves functional outcomes for patients undergoing this high-risk procedure.
The Standard highlights a range of systems and pathways health services can use to support clinical care in key areas.
Rapid assessment and escalation
- Establish systems for rapid assessment and escalation of patients with symptoms suggestive of time-critical intra‑abdominal conditions, and prompt referral for surgical review.
- Use a sepsis pathway and train staff to identify and act on sepsis.
Identifying high-risk patients
- Ensure consistent and standardised use of preoperative risk and frailty assessments; and use them to support discussions between clinicians, patients and families and to help guide their care pathways.
- Enable prompt access to theatre. Ensure the presence of a consultant surgeon and consultant anaesthetist for high-risk patients.
- Establish routine consultation about post-operative critical care for high-risk patients, and prioritise access when critical care is necessary.
Risks and goals of care discussions
- Provide support for clinicians to discuss and document patients’ goals of care and limitations on medical treatment, and ensure consistent use of a goals of care form.
- Ensure senior clinician involvement in shared decision-making about surgery when it is likely that an emergency laparotomy will not benefit a patient, or will be inconsistent with their goals and preferences.
- Provide clinicians with education, training and access to structured shared decision-making tools to support sensitive, clear and direct discussions about risk and prognostic issues.
Involving physicians for older patients
- Establish suitable local systems to support collaborative management with an appropriate physician (such as a geriatrician) with skills in the care of older patients.
Using the indicators in the Standard will support health services to identify gaps, understand what quality improvement measures are needed, and to track change.
Importantly, the indicators used in the Standard are aligned with ANZELA-QI, meaning health services that adopt the Standard and also choose to participate in the clinical quality registry will be able to compare themselves with similar services nationally.
**************************************************
A chance to improve outcomes for patients
As Australia’s first national standard for emergency laparotomy, the new Clinical Care Standard is an opportunity for Australia to experience the improvements in care that similar initiatives have achieved internationally.
In the United Kingdom, for example, the National Emergency Laparotomy Audit (NELA) has been credited with substantial improvements in emergency laparotomy outcomes, including a reduction in the mortality rate of more than 30% in its first 10 years.
It is the Commission’s intention that the Standard supports clinicians and health services to provide care that patients want and need, improve clinical decision-making and unwarranted variation, reduce the risk of complications, and lower readmission rates.
As an emergency doctor who understands what it’s like to care for a deteriorating patient and their distraught family, I urge all health services to make use of this Standard to improve pathways of care as we have for other time-critical presentations.
1. Lower-risk emergency surgical procedures, such as appendicectomy and cholecystectomy, are not covered by the Standard. Trauma laparotomy and vascular, gynaecological and urological emergency procedures are also excluded.
**************************************************
Supporting case study: using data to improve perioperative care in regional WA
Bunbury Regional Hospital acts as a regional resource centre for the entire south-west of Western Australia and performs about 15 emergency laparotomies a month.
Like other rural and regional hospitals, it must negotiate challenges such as distance, limited resources and a high-churn workforce when providing emergency care for time-critical high-risk conditions.
Despite this, since it began examining emergency laparotomy data at regular clinical review meetings, the hospital has significantly improved its performance against ANZELA-QI’s key indicators of emergency laparotomy care, and has one of the lowest crude mortality rates in Australia.
A key area of improvement has been clinicians’ use of clinical frailty assessment and mortality risk scores to help inform perioperative care pathways such as post-operative admission to ICU, and to help senior clinicians when discussing difficult decisions with patients and families.
The hospital now considers these practices business as usual. As a result, decisions about post-operative care have improved and surgery that does not align with patients’ goals of care is rare.
Dr Jacinta Cover, general surgeon and Head of Department and Medical Co-Director for Surgical, Paediatric and Maternity Services, says these practices have become the accepted way of working in the department.
“Our registrars know they can’t call me at 2 am about doing a laparotomy unless they already have these scores,” she says.
“Regularly going through that data cycle and looking at the improved outcomes overall for the patients has brought everybody on board; it’s a standardised process in our department.”
The health service has also improved emergency theatre access by confining elective surgery to certain hours of the day. It uses data to predict recovery and ensure there is access to critical care for those who are likely to need it.
“From a patient journey point of view, it means there is much less consultant-led variation in the journey. Using ANZELA-QI has really helped us to standardise our approach,” Cover says.
**************************************************
Clinical Care Standards are developed by the Australian Commission on Safety and Quality in Health Care. Their use and applicability for hospitals assessed to the National Safety and Quality Health Service Standards is described in this fact sheet on Applicability of Clinical Care Standards: www.safetyandquality.gov.au/publications-and-resources/resource-library/fact-sheet-11-applicability-clinical-care-standards.
Find out more about the Emergency Laparotomy Clinical Care Standard on the Commission’s website: www.safetyandquality.gov.au/el-ccs.

Pulse technology promises an atrial fibrillation treatment upgrade
A private hospital has been using pulse technology that has promise to treat Australia's most...
Can seasonal influenza vaccination prime the immune system for future strains?
A study analysing 30-year-old influenza-vaccinated blood samples is the first, researchers say,...
National Pain Alliance launched to advocate for chronic pain
To advocate for chronic pain to be formally recognised within national health data and policy...




![[New Zealand] Transform from Security Awareness to a Security Culture: A Vital Shift for SMB Healthcare — Webinar](https://d1v1e13ebw3o15.cloudfront.net/data/89856/wfmedia_thumb/..jpg)
![[Australia] Transform from Security Awareness to a Security Culture: A Vital Shift for SMB Healthcare — Webinar](https://d1v1e13ebw3o15.cloudfront.net/data/89855/wfmedia_thumb/..jpg)



